Cancer
What is cancer?
Cancer is a condition wherein abnormal cells grow in an uncontrolled manner throughout the body. These cells grow because the normal’s control mechanism has stopped working, and old cells stop dying and grow out of control to form new, abnormal cells. These new cells often create a tumor, which is a mass of tissue. Cancer can occur due to a number of factors, including genetics, age, and environmental risks like carcinogens.
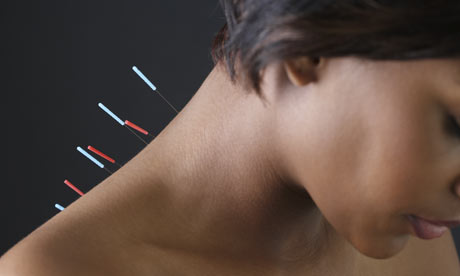
How can acupuncture and Oriental medicine help treat cancer?
Oriental medicine and acupuncture address the cancer patient as a whole, and the treatment will be specialized to the needs of the patient, rather than the prescribed recommendations of the medical community. The focus for acupuncture and Oriental medicine is to relieve the pain a patient may be going through, which can improve a prognosis exponentially. Many patients with cancer, especially those with late-stage or terminal cancer, choose to undergo Western treatment and Oriental medicine at the same time to find a balance between their benefits.
Where does Western medicine’s approach to cancer treatment fall short?
There are many productive aspects of traditional Western medicine, especially when it comes to treatment of cancer. However, Western approaches to treating cancer can be counterproductive, as well as a limitation on therapeutic approaches. The ongoing fear of malpractice lawsuits can keep medical doctors from offering treatments that can help a cancer patient heal in alternative ways, particularly in the case of late-stage or terminal cancer patients. Western medicine often treats all patients in the same way, offering the same treatment for patients in varying states of conditions, without emphasizing communication between the doctor and patient.
If you have been diagnosed with cancer and are looking for help in finding treatment, make an appointment with 120 Acupuncture Clinic today.
Related Content
Overcoming Metastatic Cancer with an Integrated Approach: A Patient’s Success Story
Over the past 20+ years, we’ve been lucky to help many people in their fight against cancer with the power of acupuncture and Oriental medicine. Let’s take a closer look at one of our patients who beat cancer and enjoys a healthy, cancer-free life today.
The Benefits of Acupuncture for Cancer Care
Many people are turning to complementary therapies to support their recovery and overall well-being during treatment and remission. Among these, acupuncture for cancer stands out as a gentle, yet powerful technique that has shown promising results through research and countless success stories. Read on to learn the many benefits of acupuncture for cancer care.
How to Manage Cancer Pain Naturally
For those looking for a more holistic approach to managing their pain and other cancer symptoms, there’s good news: acupuncture and other natural therapies can help subdue your pain while also improving your body’s chances of healing and well-being from the root.
The Perils of Smoking | Saving Your Lungs with Acupuncture
The effects of smoking on your body are broad and potentially severe. Smoking harms nearly every organ in your body, causing many diseases, and reducing one’s general health. Smoking impacts your cardiovascular system and can cause cancer to many parts of your body....
Cancer
Cancer patients don’t die directly from the cancer? If fire broke out in a building, there would be more casualties from the inhalation of poisonous gas than ones from the fire itself, victims got panic ran around to exit the smoking building without proper measures...